Let’s cover ostomy nutrition and the importance of knowing about the good and the bad out there. Of course, a low residue diet is recommended for approximately 6 weeks following ostomy surgery. For the first six weeks the stoma will be edematous (swollen) and undigested or bulky foods passing out of the stoma may cause some discomfort. Secondly, a low residue diet is restrictive of plant fibers, for instance, raw fruit and vegetables. Surely, a good rule of thumb is that if you cannot cut the fruit or vegetable with the side of your fork; you should not include it in a low residue diet. Furthermore, a soft banana can be included; an apple cannot be included. Finally, these are some ostomy nutrition tips to keep in mind after surgery.
Once the stoma swelling has subsided foods can be reintroduced slowly. It is recommended that a small amount of previously restricted food be tried. As a result, if no bloating or discomfort is noted, this food can now be included in your diet. Most foods can be eaten without problems if chewed well and eaten slowly. Evidently, if certain foods caused you problems before your illness they may again cause you problems. Ultimately, these are some tips to keep in mind while dealing with ostomy nutrition.
High Ostomy Output
When the amount of the ostomy output is high and if the texture is more like water than a thick consistency, you can try foods that can thicken the drainage. Hence, some suggested foods include:
• Breads
• Applesauce
• Crackers
• Rice
• Pretzels
• Pasta
• Peanut Butter
• Bananas


Fluids and Ostomy
If you are emptying your pouch more frequently than normal, evidently, this may be a sign that you could become dehydrated. Other signs include: lower urine output, dark yellow urine, thirst, and dry mouth and skin, for instance.
Do not just take more fluids; you must take foods that can work with the fluid to re-hydrate your system. Consequently, if you are noting signs and symptoms of dehydration, eat a starch based product (crackers, pretzels, pasta, bagel, etc) with all of the fluids you drink. As an example, eat crackers with a cup of water.
Hence, drinking alone without the inclusion of a starch based product can lead to additional liquid to exit the stoma.
Food Chart - Troubleshooting
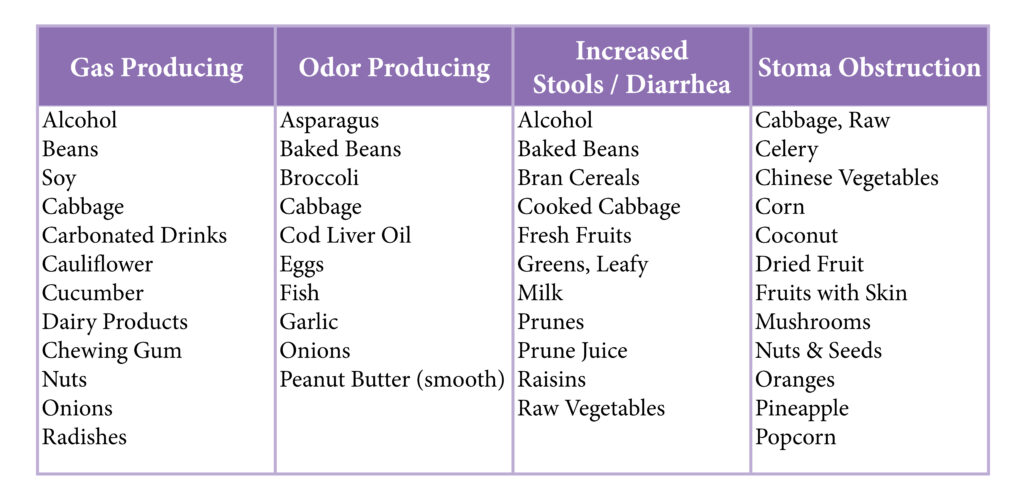
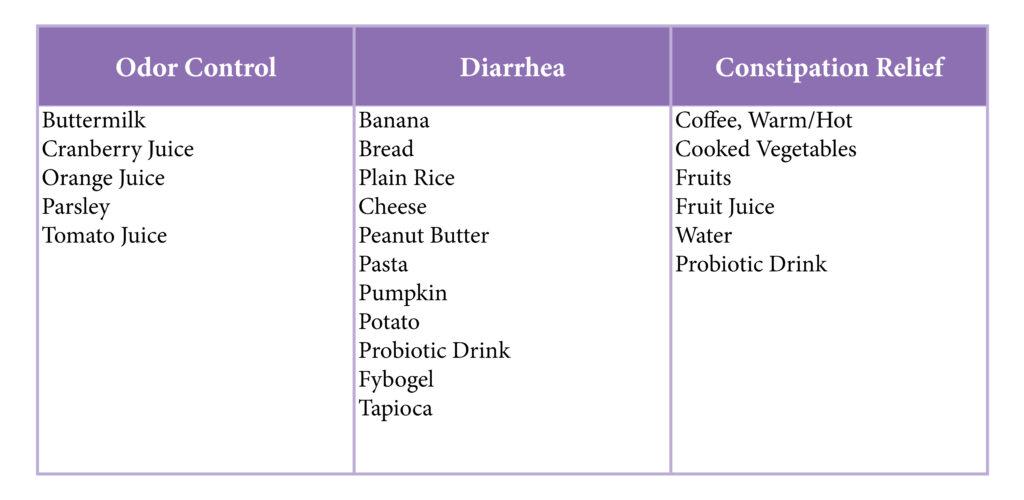
Tracheostomy Nutrition
After having a tracheostomy surgery, you likely will have a feeding tube in your nose or through the belly directly into the stomach (a gastrostomy tube) for ostomy nutrition until you are able to eat by mouth. As a result, you will need careful re-training of chewing, swallowing, and coordination of breathing to eat with a trach in place. Consequently, this can take weeks to months to learn. Once healed from surgery, your provider will tell you when it is safe to advance your diet to take in solids and liquids by mouth. Speech therapists and nutritionists can often help this process.
These tips may help with swallowing problems:
• Keep mealtimes relaxed.
• Sit up as straight as possible when you eat.
• Take small bites, less than 1 teaspoon (5 mL) of food per bite.
• Chew well and swallow your food before taking another bite.
If your tracheostomy tube has a cuff, the speech therapist or provider will ensure the cuff is deflated during meal times. Surely, this will make it easier to swallow.
For those who have a speaking valve, you may use it while you eat. For this reason, It will make it easier to swallow.
Suction the tracheostomy tube before eating. This will keep you from coughing while eating, which could make you vomit.








